Their title is just three letters, but the job of a PSW is anything but simple. Especially if you consider that, increasingly, the task of keeping people out of costly hospital visits in an already strapped healthcare system has fallen largely to them.
A Personal Support Worker (PSW) is a caregiver who helps clients with everyday life activities that – if it weren’t for physical or mental limitations – the person would normally do themselves. Things like bathing, getting dressed, feeding and going to the bathroom.
“PSWs are absolutely vital,” says Eric Mariglia, Director of Public Affairs at WoodGreen Community Services, which employs 165 personal support workers in both assisted living facilities and in the community.
▶️See what WoodGreen offers for personal support services
“They deliver the day-to-day care that allows seniors, those with disabilities and anyone who needs that type of personal supportive care, to remain in their homes and communities instead of hospitals and nursing homes”
The most recent figures estimate there are 100,000 PSWs in Ontario. And yet it is this group, arguably the largest in the health care sector, that is playing a crucial role in keeping Ontario’s health care system afloat.
Hospitals crowded with many awaiting home care
“Without PSWs, people wouldn't be able to stay where they are,” says Mariglia, who previously worked in Policy and Government Relations with the Ontario Community Support Association.
This idea of ‘aging in place’ is a key component of keeping hospital beds open for those who really need to be in hospital while also keeping taxpayer costs down. On average there are almost 5,000 alternate level of care (ALC) patients in Ontario hospitals. That means they don’t actually need the intensity of care of a hospital setting. One in 11 of those patients is waiting for home and community care services including some essential services that PSWs can provide.
“Within all three sectors: hospital, long-term care and home and community care, PSWs are vital to assure that the system stays in place and that people can have the care they need to remain healthy and well.”
At the same time as they’re providing clients with the mental health benefits of remaining in their homes, PSWs ensure that those clients aren’t left with nowhere to turn but hospitals, or prematurely in long-term care. That spells a small bit of relief for the province’s healthcare system, both in terms of patient volumes and monetary costs.
Creative, cost-saving solutions for care
By 2031, a quarter of all Canadians will be seniors over the age of 65 and 1.2 million Ontarians will need home care.
Mariglia says it’s one of the reasons the sector needs to be creative in how it delivers care in the coming years, and a driving factor behind WoodGreen’s unique cluster care model.
Cluster care brings together eight to 11 seniors with complex needs to live in shared living spaces. Each senior has their own private studio apartment with a common living and dining area for socialization. PSWs are on-hand 24 hours a day to provide care and assistance. That includes all essential activities needed for an individual to remain at home, as well as things like grocery shopping, meal preparation, laundry.. This cost-effective model allows clients to continue living in the community while also alleviating pressure on hospitals.
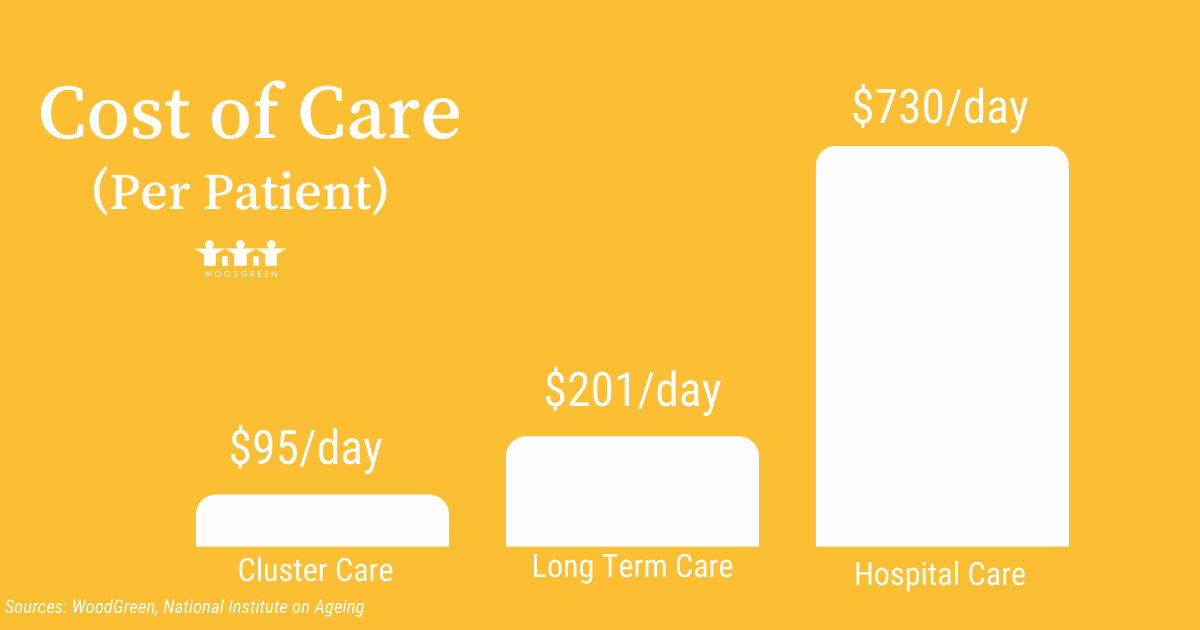
Caring for a client in cluster care costs $95 per day. That same client in a long-term care facility costs $201 per day. If that individual had no option other than to go to hospital, taxpayers would pay $730 per day for that care.
The potential cost-savings to the province of these creative care models are immense. However, Mariglia says they will only work as long as there are enough PSWs to staff them.
At every turn, he says, the PSW is the backbone of the health care system, working every day to ensure the province’s most vulnerable can live full lives with safety and dignity.
▶️Meet some of our WoodGreen PSWs.





